Beating measles with toilets – the Swachh Bharat Mission
... and what it teaches us about public health
A paper published in BMJ Open in April 2022 has found that an increase in the number of households that have toilets is associated with a decreased number of cases of measles in Indian children.
The first question that might pop into your head upon reading this is probably “What do toilets have to do with measles?”
I’m glad you asked.
As every student of public health learns, by far the largest percentage of the precipitous declines in death rates from infectious diseases that occurred in the twentieth century, was accrued long before there were any effective medical interventions. Tuberculosis, whooping cough, scarlet fever, typhoid, diphtheria and measles had all but disappeared as causes of death in Westernised countries, long before antibiotics, toxoids and vaccines were developed to treat or prevent them.

And the case definition of poliomyelitis was changed after the polio vaccination campaign began, such that the apparent steep decline in polio mortality after widespread vaccination was largely artefactual; cases of paralysis that were previously attributed to “polio” were now classified as aseptic meningitis and coxsackievirus infections.
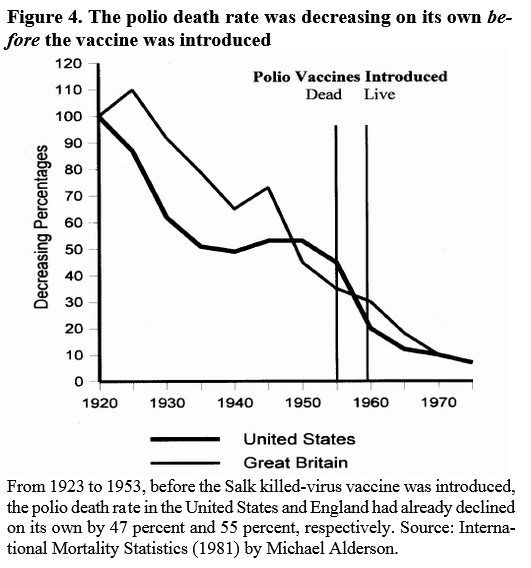
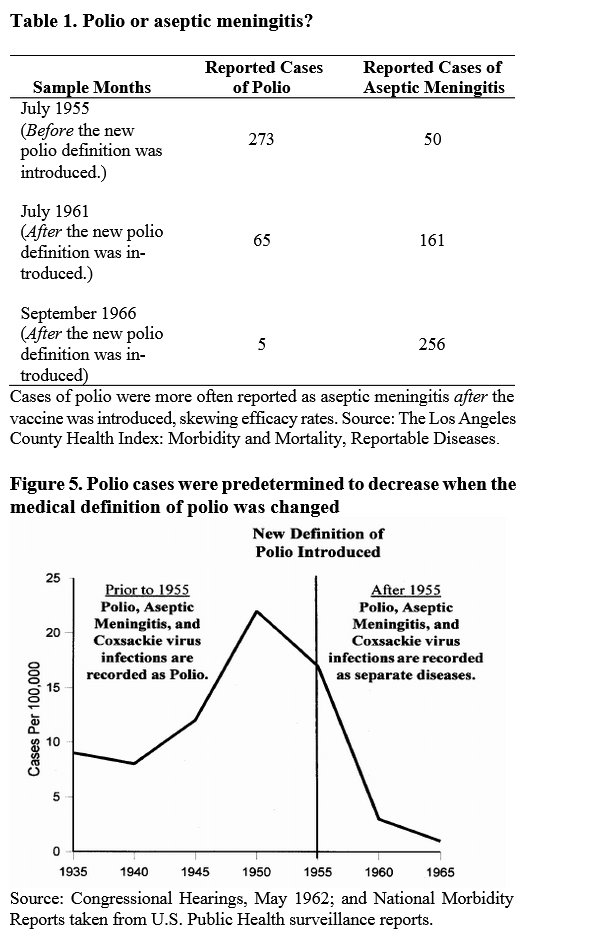
It wasn’t the miracles of modern medicine that largely eradicated the scourge of infectious diseases from industrialised countries – it was first-generation public health measures including slum reforms, food and factory inspections, and most importantly, sanitary engineering to safely remove and treat human waste and provide clean water. We have plumbers, not doctors, to thank for the fact that couples were finally able to raise families without the constant dread that they would lose several of their children to infectious disease.
Although the role that toilets play in reducing the risk of diarrhoeal disease is obvious, the effect of safe removal of human waste on a respiratory virus such as measles is far less intuitive.
However, the authors of the recently-published paper explain the link concisely:
“Improved sanitation in a community may play a role in strengthening children’s immune response.5 Owing to lack of toilets and the widespread practice of open defecation [passing bowel movements in open spaces and waterways], India serves as a unique case study.6 7 Over 60% of the global population that practices open defecation lives in India.6 7 Prolonged exposure to faecal pathogens may cause environmental enteropathy.8 This condition, or syndrome, includes nutrient malabsorption in the small intestine, atrophy of intestinal villi, crypt hyperplasia, T-cell infiltration and inflammation of the jejunum.”
In laymen’s terms, eating and drinking bacteria derived from human poop causes gut inflammation, malnutrition and impaired immunity, making children more susceptible to infectious illnesses including measles.
India has been the target of Western ‘philanthropy’ for many decades. Most notably, the Bill & Melinda Gates Foundation began working in India in 2003. The Foundation claims “to address a wide range health and development challenges, including maternal and newborn health, immunization, family planning, nutrition, and communicable diseases.”
BMGF goes on to claim that
“All of our health-related efforts and investments in India support the priorities of the Indian government. In partnering with them, we offer our expertise and global experience and an ecosystem of partnerships in service of developing relevant, scalable, and high-impact solutions.”
Just what are these “relevant, scalable, and high-impact solutions”? Scroll down the BMGF’s brag sheet on their activities in India and you’ll find that they fund drugs, vaccines, doctor and nurse training, more drugs, more vaccines, contraception, baby formula, nutritional supplementation and food fortification, more drugs, and lots more vaccines. Always more vaccines.
In fact, vaccination coverage is nearly 80% in India, which despite being the world’s fastest growing major economy still has 25% of its population living in poverty. It’s amazing how easy it is to conjure up money for vaccination programs, whilst decent housing, plumbing, reliable power and adequate food remain pipe dreams (quite literally, in the case of plumbing) for millions of Indians.
And yet, despite the likes of BMGF helping to get jabs into more Indian arms than ever before, the country continues to be ravaged by infectious diseases, recording the highest number of diphtheria and tetanus cases of any country worldwide in 2019, and also ranking among the top 10 countries in pertussis and measles cases.
So much for those “relevant, scalable, and high-impact solutions.”
Thankfully, back in 2014, someone in the Indian government had a brainwave: why don’t we pay attention to what actually worked to eradicate infectious diseases in Westernised countries? And so, the Swachh Bharat Mission (SBM), or “Clean India Campaign” was launched, with the lofty goal of eliminating open defaecation by 2 October 2019, the 150th anniversary of the birth of Mahatma Gandhi, through building toilets.
Not the $1000 a pop (or is that poop?) solar-powered toilets favoured by the purple-sweatered Grand Poobah himself, but simple loos that are affordable for a nation still wracked by poverty.
Somewhat unsurprisingly given India’s ranking as the 85th most corrupt country (out of 180), the SBM had more than its fair share of problems, including inadequate funding for behaviour change education, inappropriate containment systems and a goodly dollop of outright fraud.
Nonetheless, it succeeded in constructing over 100 million toilets across the country by 2019, providing 500 million people across 630 000 villages with a much more hygienic means of disposing of faecal material.
The program has already paid off with a reduction in undernutrition (fewer Indian children aged under 5 suffering from growth stunting and wasting) and diarrhoeal disease, which contributes significantly to undernutrition and impaired immune function.
And now, as the BMJ Open article, shows, SBM has been found to correlate with reduced cases of measles in children under 5. The drop in measles cases is not vast – for every 1% increase in households in a district with toilets, there are 0.33 fewer measles cases per 1000 children under age 5 – but in a few short years, it appears that getting loos into homes has reduced the burden of measles more than jabbing 80% of Indian kids with two doses of measles vaccine in the first two years of life.
The authors further calculated that about 12% of this decline in measles cases is directly attributable to the drop in growth stunting, providing evidence for their contention that environmental enteropathy is a major contributor to the risk of non-gastrointestinal infectious diseases like measles.
Furthermore, their analysis indicated that availability of toilets may have enhanced the impact of vitamin A supplementation on reducing measles cases. The authors point out that “vaccine response to measles relies on vitamin A supplementation and absorption”, but it is also the case that vitamin A supplementation reduces the risk of death from measles by 87% for children under two years of age.
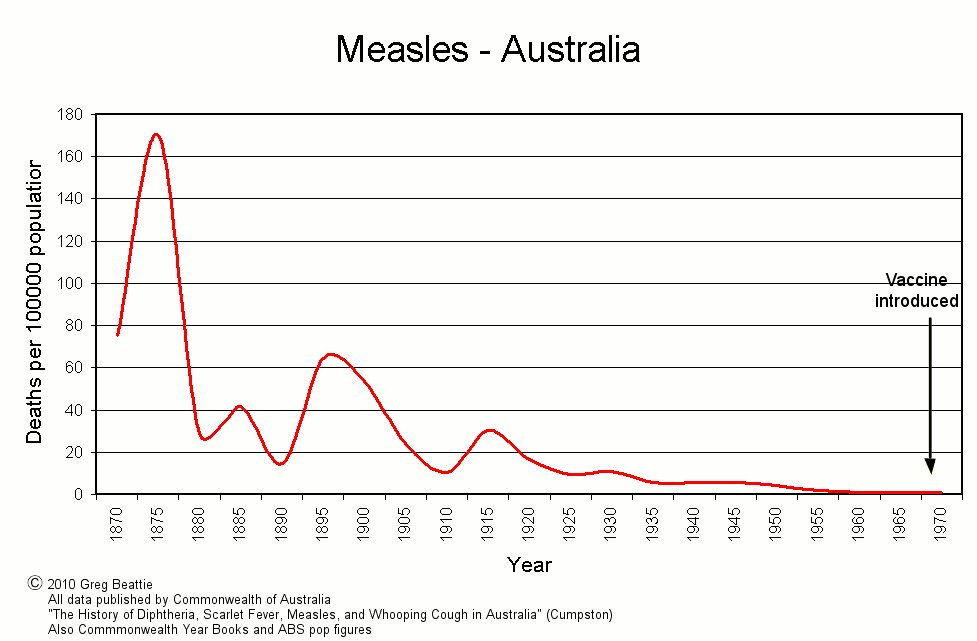
Western countries saw the disappearance of measles as a significant cause of death whilst it continued to be an endemic disease. By the middle of the twentieth century, measles was considered so unremarkable and benign that it was viewed as a childhood rite of passage, as depicted in the Brady Bunch episode ‘Is There a Doctor in the House?’, which is now considered so scandalous that you can only view it in censorship-free corners of the internet such as Bitchute:
In Australia, deaths from measles had declined so dramatically by the mid-twentieth century that measles was dropped from the national register of notifiable diseases in 1948 (meaning that doctors no longer needed to notify health authorities if they diagnosed a case of measles). It only became notifiable again in the mid-1980s when Australia embarked on a national campaign to eradicate the disease through vaccination, by which time the measles death rate was already negligible, thanks to the cumulative benefits of improved nutrition and sanitation.
The attempt to eradicate measles globally has manifestly failed, and there is growing acknowledgement that it is vaccine failure rather than failure to vaccinate that is responsible for the resurgence of measles in highly-vaccinated populations, with measles outbreaks occurring in both developed and developing countries in populations with 99%+ measles vaccination coverage.
Furthermore, acquiring measles in childhood is associated with protection against many chronic conditions. For example:
The Newcastle Thousand Families Study, a prospective cohort of 1142 individuals born in Newcastle-upon-Tyne in 1947, found that a childhood history of measles was associated with a 61% lower risk of dying of cancer during ages 15-60 years.
Getting measles in childhood was found to reduce the odds of developing chronic lymphocytic leukaemia by 43% in an Italian case-control study involving 1771 controls and 649 leukaemia cases from 11 Italian areas.
Similarly, a history of childhood measles infection was found to be associated with a lower risk of both Hodgkin and non-Hodgkin lymphoma (particularly follicular B-cell NHL).
A UK population-based case-control study found that having had 2 or more childhood infectious diseases (including chicken pox, measles, mumps, pertussis and rubella) was associated with a 55% lower risk of Hodgkin lymphoma in young adults (16–24 years).
Similarly, a population-based case-control study of San Francisco Bay area women found that having had measles before the age of 10 was associated with a reduced risk of Epstein-Barr virus-positive Hodgkin lymphoma.
Allergic diseases including dust mite allergy and asthma are less common in children who have had measles; children in Guinea-Bissau who had had measles were found to have roughly half (12.8% vs 25.6%) the risk of atopy – the tendency to produce an exaggerated immunoglobulin E (IgE) immune response to otherwise harmless substances in the environment – as children who had been vaccinated and not had measles.
The acute stage of measles infection appears to suppress the activity of the malaria parasite, Plasmodium falciparum, such that only 25% of children with measles had malaria parasites in their blood vs 88% of children without measles.
Intractable epileptic seizures have been observed to disappear following acute viral infections including measles.
A case-control analysis of Parkinson’s disease and infections in childhood conducted in a cohort of 50 002 men who attended either Harvard College or the University of Pennsylvania between 1916 and 1950 found that a history of measles prior to college entrance was associated with a 47% lower risk of developing Parkinson’s disease.
How do we thread the needle between the very real risks of serious illness, lifelong complications and death in undernourished, immunocompromised children who contract measles, and the apparent protection against multiple serious diseases of adulthood conferred by measles infection in otherwise healthy, well-nourished children?
Should we spend $US 2.3 billion per year on vaccines in a vainglorious attempt to eradicate measles from every corner of the globe? Or would that money be better spent on providing the fundamentals of public health – like toilets – to the millions of people in developing countries who lack them?
To reduce hunger and the nutrient deficiencies that increase the risk of serious outcomes of infection with measles and other childhood diseases, how about promoting traditional farming methods that increase the nutrient density of crops instead of persuading governments of impoverished nations to pour money they don’t have into Bill Gates’ vanity projects like the Alliance for a Green Revolution in Africa (AGRA), which has resulted in 30% higher rates of undernourishment in the countries which adopted his high-tech, chemical-dependent, patented seeds – which, by sheer coincidence, are produced by companies that he owns major stakes in?
And given that, after measles vaccination began in the US, the death rate from measles was found to be almost ten times higher in counties with the lowest median household income than in the wealthiest counties, why have public health authorities focused so obsessively on jabbing every last child with multiple doses of vaccines, rather than pushing for policies that close the poverty gap – and in so doing, reduce the risk of all infectious diseases as well as many chronic ones?
As I wrote in my miniseries on philanthrocapitalism and public health (Part 1 and Part 2), the public health movement has been hijacked by the profit motive – and it’s not just people in developing countries who are suffering from it.
We are at a most interesting point in history, where the abject failure of pharmaceutical solutions to COVID-19 (injections that don’t stop infection or transmission, and antiviral drugs that don’t prevent hospitalisation or death) is becoming more evident every day, while our governments continue to throw taxpayers’ money at these white elephants.
Perhaps we may take the publication in a major medical journal of a study on the infectious disease-reducing power of the humble toilet as a sign that it’s time we forced our public health authorities to euthanise the Frankenstein monster version of Big Pharma/Public Health Inc that they’ve been pushing on us, and take public health back to its roots.
And if you want to personally contribute to an initiative to provide toilets and improve sanitation in developing countries, order your toilet paper from the good folks at Who Gives A Crap, who donate 50% of their profits to doing just that. Sure beats the crap out of the Bill & Melinda Gates Foundation.





Another great article.
I don't whether it's the last two years such that many of my previously 'firmly held' beliefs have now almost turned 189 degrees, but it seems to me that there are more and more stories or articles coming out that question the existence of viruses.
Or maybe it's that I just follow or stumble across more 'conspiracy theorists'.
I let my kids play outside in the direct, and I have fond memories of them sticking rocks in their mouths. That's just nature at work. Apparently when a baby is born naturally, he or she ingests a bit of poo on their way out.
Turns out that this is a good thing, and I believe that now babies born in a caesarian manner have a bit of mum's poo smeared on their lips.
Where am I going with this ? I read another substack by a Midwestern Doctor, https://amidwesterndoctor.substack.com/p/why-do-doctors-close-their-eyes-to?r=9wy0f&s=r&utm_campaign=post&utm_medium=web&utm_source=direct who says that the healthiest oldies he encounters are the ones who don't take any medication. I think scientist try to be too clever sometimes and I agree that it's more about the money. I'd like to think that is all and not anything more nefarious, though I'm open to that.
I guess the only good thing about the 'measles vaccine' if that you can stand up and court and say that it prevents transmission (because that appears to be the consensus) unlike the latest mrna ones. Apologies for the waffle
Hi Robyn, just another quick thankyou for your articles. They are the most enjoyable read I get each week.